|
|

|
Medical Devices of the Neck & Spine continued
by Tim B Hunter, MD, MSc and Mihra S Taljanovic, MD, PhD
Thoracic and Lumbar Spine Instrumentation continued...
Anterior Spinal Instrumentation
The devices used for anterior spinal instrumentation are similar to those used for posterior spinal fixation and usually include plates and screws (Hu, 1992; Slone, 1993; Aebi, 1998; An, 1999; Benzel, 1999; Hitchon, 1995). Anterior spinal fixation is common in the cervical spine, but, as discussed above, it is uncommon in the thoracic or lumbar spine. When it is used in the thoracic or lumbar regions, it is often designed to stabilize or correct a marked kyphosis or scoliosis. The anterior spinal apparatus is placed to impart a distracting force on the concave side of the scoliosis or a compressing force on the convex side of the scoliosis. It is also useful in anterior approaches to spinal tumors or metastatic disease.
Anterior lumbar interbody fusion (ALIF) has become more popular and is a somewhat limited procedure (figure: ALIF; figure: zero-profile lumbar fixation L2-5). It offers an easy approach to the anterior disk space without opening the spinal canal or neural foramina, such as the case with posterior lumbar interbody fusion (PLIF) or transforaminal lumbar interbody fusion (TLIF). ALIF allows the placement of a large interbody fusion device and easy and complete diskectomy (Mobbs, 2013). ALIF is used for chronic back pain of discogenic origin over 1 - 3 levels.
ALIF is often performed with zero-profile systems using a low profile spacer anchored by fixation screws into vertebral bodies above and below the diskectomy level (figure: zero-profile lumbar fixation L2-5). The native disks are usually replaced with PEEK artificial disks. While ALIF is somewhat of a more limited surgery compared to several other approaches, it has the disadvantage of potential vascular or bowel injury resulting from the anterior approach to the spine. There has to be mobilization of the great blood vessels and peritoneal contents away from the spine exposing them to possible injury (Mobbs, 2013).
Lateral/posterior Spinal Instrumentation
ILIF (interlaminar lumbar instrument fusion) is a more recently introduced lumbar spine surgery for degenerative spinal stenosis which decompresses the spine and also fuses lumbar vertebrae together with donar bone placed between spinous processes and held in place by a small spinous process fixation plate or clamp (figure: interlaminar lumbar spinal instrumentation; figure: interspinous clamps at L4-5). There may also be other lumbar fusion apparatus as well.
Extreme lateral interbody fusion (XLIF) is a minimally invasive surgical procedure performed from a lateral approach to remove a diseased disk with placement of an artificial disk and performance of lateral fixation with plate and screws going into the vertebral bodies above and below the diseased disk space level (Nuvasive) (Ha, 2014; Petscavage-Thomas, 2020) (figure: XLIF). A similar procedure is the transforaminal lumbar interbody fusion (TLIF).
Oblique lumbar interbody fusion (OLIF), anterior to psoas approach (ATP), reaches the intervertebral disk between the retroperitoneum and psoas muscle. Both OLIF and lateral lumbar interbody fusion (LLIF) allow for correction of scoliosis and laterolisthesis with OLIF less likely to damage the lumbar plexus at surgery (Winegar, 2019; Petscavage-Thomas, 2020). Multiple imaging modalities have a role after lumbar fusion beside standard radiographs. Wangaryattawanich and colleagues (2020) feel CT is the preferred modality after lumbar fusion for assesing spinal hardwared complicatons, bone integrity, and status of the fusion.
Lumbar interspinous distraction devices are designed for adult patients with position dependent spinal claudication in which spinal stenosis is lessened in flexion. In some patients flexion decreases epidural pressure, increasing the relative size of foramina and the spinal canal, and decreasing nerve root compression (Ha, 2014; Petscavage-Thomas, 2020). These devices provide a localized lumbar fixed flexion by producing distraction between adjacent spinous processes through a variety of spacers placed between the spinous processes. Several evolving designs and indications for their use have been introduced in the last decade, including the X-stop device (rheumatology network), and the Coflex device (Paradigm Spine) (figure: X-stop device; figure: Coflex device).
Vertebroplasty and Kyphoplasty
Vertebroplasty is designed to provide pain relief from benign osteoporotic compression fractures or less common, destructive vertebral lesions (Cotten, 1998; Hulme, 2006; Petscavage-Thomas, 2014; McConnell, 2014). Methyl methacrylate is injected directly into a vertebral body to strengthen the bone structure of the vertebra and immobilize fractures, which provides immediate pain relief. If the patients are properly selected and the procedure goes well, vertebroplasty is a dramatic technique. Patients who are bedridden or wheelchair bound have such relief from the chronic
pain of vertebral collapse that they frequently ask to walk out of the hospital. Vertebroplasty is a
serious procedure, and patients must be carefully selected. Because the methyl methacrylate is
mixed with barium sulfate, it is visible on radiographs and on cross-sectional images (figure: vertebroplasty).
Studies in 2009 (Kallmes; Buchbinder) suggested there is little or no benefit of vertebroplasty relative to a control procedure in short term patient reported outcomes, and the use of vertebroplasty has become somewhat controversial. A more recent study with patient reported outcomes through year 1 shows vertebroplasty may provide a modest reduction in pain one year later compared to a control procedure (Comstock, 2013). A 2020 Radiology meta-analysis (Hinde, 2020) suggests vertebroplasty not only improves the quality of life for patients but also helps patients live longer. Further studies are warranted to determine which patients would benefit the most from vertebroplasty (Jennings, 2020).
A variation of vertebroplasty is kyphoplasty, which uses a balloon that is inflated in the treated vertebral body to create a cavity within the vertebral cancellous bone (figure: kyphoplasty systems). The vertebroplasty cement is instilled directly into the newly created cavity after the balloon is deflated. Kyphoplasty and vertebroplasty have similar outcomes. Kyphoplasty is somewhat more expensive, but it can sometimes restore the height of the central aspect of the vertebral body by as much as 3 mm (Petscavage-Thomas, 2014). It is sometimes used for kyphotic deformity correction or in more complex cases of vertebral injury (McConnell, 2014).
Vertebroplasty volumes and rates decreased sharply after 2009. There is a trend toward more kyphoplasty which has somewhat offset the decrease in volume of vertebroplasty procedures (Cox, 2016). The 2020 study by Hinde showed kyphoplasty outperformed vertebroplasty on mortality. This may be from improved pulmonary function as the result of restoration of vertebral height as well as possible improved mobility (Hinde, 2020).
The Kiva VCF Treatment System (Benvue) is a recently introduced approach to vertebral augmentation via vertebroplasty. It is designed for reduction and treatment of spinal fractures from T6-L5. It uses a unilateral transpedicular percutaneous approach in which a PEEK cylindrical implant is placed into the vertebral body using a guidewire The PEEK implant forms a hollow spiral tube in the vertebral body into which vertebroplasty cement is instilled. The implant and hardened cement help to restore vertebral height and remain within the vertebral body.
Vertebroplasty may employ a radiofrequency technique. Polymethylmethacrylate (PMMA)-based inject is used and activated or heated by a radiofrequency signal just prior to application. This increases its viscosity and reduces the likelihood of extravasation (Winegar, 2019).
Back to Top
| Expandable corpectomy cage |
Expandable corpectomy cage Sagittal reformatted CT image |
Expandable corpectomy cage after cage shift |
Coflex device |
 |
 |
 |
 |
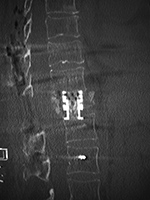
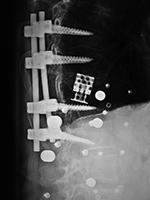
| 75-year old woman with expandable corpectomy cage used to treat a comminuted T11 compression fracture (left and center images). A follow-up study 3 months after cage placement (right image) shows cage shift probably from increased fracture compression. The cage remained stable at that point. |
The Coflex device is made from titanium. The "U" shaped device is positioned horizontally with its apex anterior. The two long arms of the "U" parallel the long axis of the spinous process. The ridges help keep the device stably attached to the spinous process. Image from Paradigm Spine |
 |
| Vertebroplasty at L1 and L3 (AP view) |
Vertebroplasty at L1 and L3 (lateral view) |
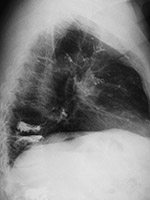
Embolization of vertebroplasty cement into the pulmonary arterial tree |
 |
 |
 |
 |
| There is extrusion of vertebroplasty cement into the T12-L1 disk space. |
There is extrusion of vertebroplasty cement into the T12-L1 disk space. |
From Hunter, 2004 |
 |
| Dorsal column stimulation unit in upper cervical spine |
Dorsal column stimulation unit in lower thoracic spine |
 |
 |
 |
 |
| There are skin staples from the recent surgery. From Hunter, 2004 |
Congenital fusion of the C5 and C6 vertebral bodies is present. From Hunter, 2004 |
AP view |
Lateral view |
 |
| TLSO (Boston) brace AP view |
TLSO (Boston) brace lateral view |
Baclofen intrathecal delivery pump AP view |
Baclofen intrathecal delivery pump lateral view |
 |
 |
 |
 |
| This brace was used to treat an L1 compression fracture |
The catheter (arrow) goes into the lower thoracic spinal subarachnoid space. |
The catheter (arrow) goes into the lower thoracic subarachnoid space. |
 |
| Intrathecal drug delivery catheter (arrow) |
Sacral stimulator AP and lateral views |
Sacral stimulator (AP view) |
 |
 |
 |
 |
| The catheter is in the lower thoracic subarachnoid space. It exits in an anterior abdominal delivery pump. From Hunter, 2004 |
|
|
This is a different patient than the preceding two images. From Hunter, 2004 |
 |
| Zero-Profile lumbar fixation L2-L5 |
 |
 |
 |
 |
| 45 year-old woman with L2-5 anterior lumbar interbody fusion (ALIF) for low back pain. The lateral views are respectively in neutral and flexion positions. The CT images are selected slices in the coronal and sagittal planes, respectively. |
 |
| Zero-Profile lumbar fixation L2-L4 |
Kyphoplasty |
|
 |
 |
 |
|
| 45 year-old woman with L2-5 anterior lumbar interbody fusion (ALIF) for low back pain. |
Vertebral Body Balloon (VBB) System (DePuy Synthes) for vertebral augmentation procedures (kyphoplasty). © DePuy Synthes 2016. All rights reserved. Vertebral Body Balloon (VBB) System is a trademark of DePuy Synthes. |
Confidence Spinal Cement System for kyphoplasty. © DePuy Synthes 2016. All rights reserved. CONFIDENCE SPINAL CEMENT SYSTEM® is a trademark of DePuy Synthes. |
|
 |
| X-stop device |
X-Stop Devices |
 |
 |
 |
 |
| Image from rheumatology network |
69 year old man with chronic low back pain treated with X-Stop devices at L4-5 and L5-S1. Sagittal T1-w MRI (3rd image) shows some metallic susceptibility artifact but the spinal canal is visible. |
 |
| Extreme lateral interbody fusion (XLIF) |
ProDisc L |
 |
 |
 |
 |
| Images from Nuvasive |
ProDisc L (Synthes) artificial lumbar disk. © DePuy Synthes 2016. All rights reserved. ProDisc® L is a trademark of DePuy Synthes. |
Back to Top
Artificial Disks; Total Disk Replacement (TDR)
Artificial disk cages are most often used concurrently with other spinal
surgery (Lee, 1991). A stand alone total artificial disk or total disk replacement (TDR) is designed to maintain a normal range of motion at a specific spinal level decreasing the risk of adjacent spine segment degeneration. These types of artificial disks are most commonly placed for degenerative disk disease located at a single level in the cervical or lumbar spine. One popular design consist of two metallic (end)plates or other hard materials
that have metallic teeth to anchor them to the vertebrae above and below the disk space. Between
the plates is a rubber core containing polyethylene to allow for motion and cushioning. A similar design can be used in other body locations, such as in the temporomandibular joints. The SB Charite III Dynamic Disc Spacer is an example of such a design.
The ProDisc C (DePuy Synthes) is for treatment of a single degenerated disk in the cervical spine (C3-7). It has a ball and socket design in which a plastic inlay is affixed to the bottom metal endplate forming the ball, and a concave metal surface in the top endplate forms the socket (figure: ProDisc C). The ProDisc L (DePuy Synthes) is for total disk replacement for the lumbar spine (L3-S1) (figure: ProDisc L). The Prestige Cervical Disc (Medtronic) has a ball and groove design using a cobalt chromium alloy metal-on-metal articulation around the center of an elliptical ball. Other artificial cervical disks are the Bryan Cervical Disc System (Medtronic), the Mobi-C Cervical Disk (LDR Holding Corporation), and the Secure-C Cervical Artificial Disk (Globus Medical) (figure: Secure-C Cervical Artificial Disc). All of the total disk replacement devices have associated complications, including subsidence, particle disease, dislocation, vertebral fractures, infection, heterotopic ossification, and adjacent spinal degeneration above and below the artificial disk level (Petscavage-Thomas, 2014).
Generically, these types of total disk replacement systems are called "metal-on-polyethylene" disks (figure: metal-on-polyethylene cervical disk). The liners in these disk prostheses are usually designed to float or shift on the anchored metallic inserts. Sometimes, the liners, which are radiolucent, have a metallic circumferential ring for their identification on radiographs (figure: lumbar spine L4-5 total disk replacement; figure: lumbar spine fusion and disk replacements). As with all other types of medical apparatus, knowing the exact brand name is nearly impossible and not important. What is important is realizing the presence of the artificial disk, noting whether it is properly positioned and whether it shows any sign of complication.
Threaded bone dowels may also be used instead of artificial disks or vertebral cages. They are made from human allograft bone and are designed to provide a support system for new bone formation (figure: cervical bone struts; figure: intervertebral disk spacer).
Back to Top
Adjacent Segment Degeneration (Disease); Junctional Disease
Successful spine stabilization surgery eliminates motion at the diseased segment, but it often significantly increases biomechanical stresses on adjacent non-fused segments of the spine, typically those cephalad to the fused segment. This increased biomechanical stress over time may result in fairly rapid degeneration of the segment cephalad (and sometimes the segment caudad) to the fused region with disk degeneration, degenerative spondylolisthesis, instability, hypertrophic facet arthropathy, disk herniation, and spinal canal stenosis (Winegar, 2019) (figure: cervical spine adjacent segment disease).
Adjacent segment degeneration represents the radiographic appearance of these biomechanical changes above or below a region of surgical spinal instrumentation and fusion, no matter the part of the spine-cervical, thoracic, or lumbar. If there is overt symptomatology from this rapid postoperative degenerative spine disease, the term advanced segement disease (or junctonal disease) is used, though the difference between "change" and "disease" may be more semantic than actual. One of the main goals of modern spine surgery and spinal fixation apparatus is to ameliorate or eliminate this frequent after effect of spine stabilization surgery. It is not uncommon for further spinal surgery to be performed to treat adjacent segment disease. Devices designed to address this complication alone or in tandem with other devices include artificial disks, special posterior stabilization apparatus, interspinous spacers, and facet joint arthroplasties (Winegar, 2019).
Back to Top
|