Orthopedic Devices
|
|
Internal Fixation - pins, wires, and screws |
|
|
|
|
|
|
|
|

|
Fracture Fixation continued...
by Tim B Hunter, MD, MSc
Internal Fixation...pins, wires, & screws
Since the late 1950s, open reduction and internal
fixation (ORIF) has been used to treat fractures. It enables rapid restoration of bone
anatomy and early patient mobilization to
overcome the limitations encountered when fractures
are treated with skeletal traction or cast immobilization
(Ruedi, 2007; Benjamin, 1994; Freiberg, 2001; Hunter, 2001).
The main goal of internal
fixation is the achievement of prompt and, if possible,
full function of the injured limb, with rapid
rehabilitation of the patient. The majority of internal
fixation implants are currently made of stainless steel. Occasionally, less strong but biologically
superior and more elastic titanium implants
are favored.
Numerous devices are available
for internal fixation. These devices can be
roughly divided into a few major categories: a) wires, b) pins and screws, c) plates, and d) intramedullary
nails or rods. Staples and clamps are also used
occasionally for osteotomy or fracture fixation
(Ruedi, 2007; Benjamin, 1994; Wiss, 2013; Berquist, 1995; Freiberg, 2001; Hunter, 2001; Parker, 2002; Stover, 2001; Craig, 2001).
Pins
Fixation pins come in many designs and sizes and can be smooth or
threaded.
Among the most commonly used fixation pins are Kirschner (K)-wires (figure: pins in plaster; figure: K wires) and Steinman pin (figure: uniplanar external fixator with Steinman pins; figure: Steinman pins stabilizing left humerus fracture). These devices
are mainly used for temporary fixation of fracture
fragments during fracture reduction or to attach
skeletal traction devices. Sometimes, they act as guides for
the accurate placement of larger cannulated screws.
Percutaneously placed Kirschner
wires commonly protrude through the skin for
ease of later removal. Occasionally, pins are
used for definitive fracture treatment and should
be especially watched for migration. The Steinman pin is
also occasionally used for wrist arthrodesis (Jebson, 2001). On rare occasions pins may be used for other applications, such as tendon reconstruction or lengthening (figure: Achilles tendon lengthening pin).
It should be noted the terms pins and wires are commonly used interchangeably and inconsistently. Pins are more often thought of as straight thin metallic rods typically inserted so as to retain their straight form. However, they can be cut and bent for a given treatment situation. Wires are most often though of as thinner metallic rods easily bent and shaped similar to common wire used around the house or in the garden. Cables and bands are larger more rigid wires.
Wires
Wires are sometimes used alone but more commonly in combination
with other orthopedic fixation devices.
They are of various diameters and can be braided.
Wires are frequently used to reattach osteotomized
bone fragments (i.e., the greater trochanter to the femur or
the olecranon process to the ulna). In combination with pins or screws, wires are sometimes used to create a tension band, which
uses distractive muscular forces to create compression
at the fracture site (figure: olecranon fracture fixation) (figure: patellar tension band wiring).
Wires are
used to suture bone and soft tissue, and they occasionally break (figure: broken trochanteric wire). However, if there is no loss of bone fragment
position, breakage of wires is usually of little
significance. Circumferential cerclage wires are
commonly used in conjunction with intramedullary
fixation to stabilize long bone fragments and stems of prostheses or fixation plates (figure: femur cerclage wires). One of the potential complications with cerclage
wires is interruption of the periosteal blood
supply with subsequent osteonecrosis or fracture
nonunion (Ruedi, 2007; Benjamin, 1994; Wiss, 2013; Berquist, 1995; Freiberg, 2001; Hunter, 2001).
Screws
A variety of screws are used in everyday orthopedic practice. The main parts of a screw are the screw
head, which is its bulbous end and the part engaged
by the screwdriver, and the shank or core,
which can be of variable diameter and is partially
or fully threaded. The distance between the
threads is called “pitch” (figure: anatomy of a fixation screw).
Screws are of
different sizes and can be self-tapping (which
have cutting ends) or non-self-tapping. Non-self-tapping
screws are easier to insert and remove,
but they are not the best choice for fixing fractures
in regions with a thin cortex. Some screws
have a “standard” point and others a “trocar” point. Screws are commonly used in combination
with plates and nails or rods. The use of different
types and designs of screws depends on the surgeon’s
preference (Ruedi, 2007; Benjamin, 1994; Wiss, 2013; Berquist, 1995; Freiberg, 2001; Hunter, 2001).
There are two basic types of fixation screws,
cortical and cancellous, according to the Arbeitsgemeinschaft fur Osteosythesefragen - known to English-speaking countries
as the Association for the Study of Internal Fixation [ASIF]. Cortical bone screws are often fully threaded and usually
have a smaller thread diameter and pitch (figure: cortical and cancellous fixation screws). Cortical screws are designed to be used in
the diaphysis.
Cancellous bone screws are intended to
cross long segments of cancellous bone. They
typically have deeper threads, larger thread diameters,
and a greater pitch than cortical screws. Cancellous screws are usually partially threaded with threads
only on their ends (figure: olecranon cancellous bone screw; figure: hip cannulated cancellous screws). Occasionally, cancellous
screws can be fully threaded (Ruedi, 2007).
Schanz screws have a larger
core diameter and less deep self-cutting threads,
which provides better buttressing against forces
that act perpendicular to the long axis of the
screw (figure: uniplanar external fixator). There are other types of diaphyseal unicortical locking screws that are used with plates to provide better
anchorage and which can function as a fixed angle device (Ruedi, 2007).
A screw that crosses a fracture line (ideally,
perpendicular to the fracture line) is called an “interfragmentary” screw or "lag" screw. This screw provides compression between the
fracture fragments to enhance fracture stability
and promote healing. Sometimes a lag screw is more specifically defined as an interfragmentary screw with a gliding hole in
the near (cis) cortex and a threaded hole in the far
(trans) cortex.
Fully threaded cortical interfragmentary
screws are used in the diaphysis of bones, because they are
easier to remove than partially threaded cancellous
screws. Sometimes, an interfragmentary
screw is placed through a fixation plate. Interfragmentary screws are preferred in the fixation of
articular fractures to obtain anatomic reduction
and adequate stability. Interfragmentary screws are also preferred for treating juxtaarticular fractures.
Self-tapping screws, which have cutting
ends, are not recommended for use as interfragmentary screws
because removal and reapplication of the screw
may be needed. Interfragmentary screws are used
occasionally to treat open fractures (i.e., in case of
very long oblique spiral fractures or in the presence
of a large well-vascularized third fragment
that requires fixation) (Ruedi, 2007; Benjamin, 1994; Berquist, 1995; Freiberg, 2001; Hunter, 2001).
In certain situations, a washer (metallic ring) is
used with a screw to prevent the screw head
from sinking into the bone. Washers enhance
the compressive area of a screw in regions of thin cortex, and they prevent fractures under
the screw (figure: dynamic hip compression screw with cannulated fixation screw and washer).
Loosening of well-placed screws is induced by
micro motion at the interface between the thread
and bone. From a radiologic standpoint, it is important
to observe and report possible complications
including screw breakage, loosening, or
change in position (Ruedi, 2007; Benjamin, 1994; Hunter, 2001). A screw that is used to stabilize the distal tibiofibular
syndesmosis is called a syndesmotic screw.
This screw is placed across the distal tibiofibular
joint parallel and 1–2 cm proximal to the joint
line. One or more syndesmotic screws can also be placed
through the holes of a fibular fixation plate (figure: syndesmotic screws; figure: syndesmotic screws and medial malleolus cortical screws).
Syndesmotic screws are usually removed 6 –12
weeks after placement, after the interosseous
membrane has healed (Ruedi, 2007; Benjamin, 1994; Berquist, 1995; Freiberg, 2001; Hunter, 2001).
Cannulated screws have a hollow shank, which
allows them to be placed more exactly over a
guide pin (figure: cannulated screw). They are commonly used for fixation
of subcapital hip fractures and may be inserted
percutaneously with fluoroscopic guidance (figure: hip cannulated screws). This surgery is commonly performed by
using a fracture table to provide traction and
maintain reduction during the fixation (Ruedi, 2007; Benjamin, 1994; Berquist, 1995; Freiberg, 2001; Hunter, 2001).
A special type of screw used in the treatment
of intertrochanteric proximal femur fractures
is called a dynamic compression screw (device) consisting of a large lag screw with
distal threads that is inserted into the femoral
head and neck. This screw fits into the barrel of a
side plate, which is secured to the femoral shaft
with multiple cortical screws. The lag screw can
slide within the barrel, which results in compression
of the fracture site as the patient ambulates (figure: hip dynamic compression screw)
(Ruedi, 2007; Benjamin, 1994; Berquist, 1995; Freiberg, 2001; Hunter, 2001). If the fracture settles, the lag screw slides within the barrel preventing the screw from piercing the femoral head and entering the hip joint space.
Large spiral or helical screws are sometimes used to secure femoral neck fractures, acting as a dynamic compression screw. This design is also used in other circumstances, such as a distal locking screw placed in an intramedullary rod (nail) (figure: blade spiral distal locking screw).
Another “special” screw is a Herbert screw,
which was originally designed for the fixation of
scaphoid fractures (figure: Herbert screw). Currently, this screw has a
more broad application. The Herbert
screw has threads of different pitch at both ends,
with an unthreaded central shank. It does not
have a head. It acts as a countersink, allowing different
threads at its ends to draw the fracture fragments
together (Ruedi, 2007; Benjamin, 1994; Hunter, 2001; Herbert, 1984). It is sometimes said to have cancellous threads on one end, while the other end has a larger diameter with cortical threads.
A similar screw is the Acutrak screw. It is headless with variable thread pitch on either end, but it does not have an unthreaded central shank (figure: Acutrak screw) (figure: Acutrak screws and endobuttons). It is very commonly used for the treatment of finger and wrist fractures. The Smart (toe) implant is a product of Stryker specifically designed for interdigital fusion of fingers or toes and other small bones. It is sometimes used in conjunction with K-wires and small fixation screws (figure: Smart toe implants).
For capsular, tendinous, and ligamentous repairs,
a variety of anchor screws (suture anchors) are used (figure: suture anchors in glenoid rim; figure: suture anchor in humeral head).
These screws have barbs and hooks for soft-tissue
or bone attachment and allow for suturing of ligaments
to the anchor, which is then placed in the
bone (Ruedi, 2007; Benjamin, 1994; Hunter, 2001).
Other devices used for soft tissue anchoring are Endobuttons. An Endobutton is a cortical bone fixation device with a continuous loop suture and no fixation knot (figure: endobuttons). Endobuttons were designed for anterior cruciate ligament reconstruction and fixation but are also used for other ligamentous repairs (figure: ACL reconstruction with bioabsorbable interference screw and endobutton; figure: thumb endobuttons) (Melville, 2015). There is direct fixation of the repair graft onto a small metallic button like device through which continuous loop suturing is used with the fixation device secured directly to the external surface of cortical bone.
Fixation techniques for anterior cruciate ligament
(ACL) grafts continue to evolve (figure: ACL ligament substitute). The Kurosaka screw, which is also called an interference screw,
is designed to anchor the ACL graft into the lateral
femoral condyle and proximal medial tibial
metaphysis bone tunnels (Kurosaka, 1987) (figure: ABSOLUTE and Biosure interference screws; figure: interference (Kurosaka) screw). This screw is headless, short, and
broad. There are a variety of designs for interference
screws that act as anchors for the fixation of
ACL grafts (Beevers, 2003; Pena, 1996). These screws can be metallic or bioabsorbable
and radiolucent (figure: interference screw). Aside from interference screws, there are other
devices used for the fixation of the ACL graft, including buttons, washers, staples, cross pins,
polyester titanium buttons, and suture posts (figure: ACL repair with bioabsorbable interference screw and Endobutton).
The radiographic appearance of the knee after
ACL reconstruction is usually initially evaluated with standard radiographs (Manaster, 1988). On the lateral radiograph,
the tibial osseous tunnel should begin distally
near the tibial tuberosity, course posteriorly, and
exit the tibial articular surface immediately anterior
to the anterior tibial spine. On the frontal radiograph,
the tibial tunnel begins in the medial
tibial side, courses laterally and proximally, and
exits the articular surface at the intercondylar
eminence of the tibial plateau.
The appropriately
placed ACL graft has an oblique orientation and
on sagittal oblique magnetic resonance images is
posterior to the intercondylar roof line (Blumensaat
line). On the lateral radiograph, the femoral
osseous tunnel extends from the intersection of
two lines, which represent the posterior femoral
cortex and the intercondylar roof. On the frontal
radiograph, the femoral tunnel begins laterally,
just superior to the lateral femoral condyle, and
emerges on the superolateral aspect of the intercondylar notch. Once standard radiographs have been obtained, the
integrity and possible complications of the ACL
graft are evaluated frequently with magnetic resonance
imaging (Martin, 2002; Resnick, 2007).
Back to Top
| Uniplanar external fixator with Steinman pins |
Tension band wire |
Broken trochanteric osteotomy wire |
Cerclage wires |
 |
 |
 |
 |
| The unilateral pins just penetrate the far cortex and are connected with radiolucent rod. The fixator is immobilizing a tibial fracture. From Benjamin, 1994 |
Tension band fixation of an olecranon fracture using a cancellous screw. The looped wire transforms the distractive pull of the triceps into compression at the fracture site. From Benjamin, 1994 |
A cemented total hip arthroplasty has a trochanteric osteotomy fixed with wires. The wire is broken laterally. The arrows point to evidence of polyethylene wear in the acetabulum. From Benjamin, 1994 |
A long stem bipolar hip prosthesis has cerclage wires in the diaphysis of the femur. From Benjamin, 1994 |
 |
| The anatomy of a fixation screw |
Cancellous and cortical bone screws |
Hip cannulated cancellous fixation screws |
Hip dynamic compression screw set |
 |
 |

|
 |
| From Benjamin, 1994 |
From Benjamin, 1994 |
|
1- lag screw; 2-compression screw; 3-barrel and side plate. From Benjamin, 1994 |
 |
| Cannulated screw with threaded-tipped guide pin and Herbert screw |
Cannulated screws |
ABSOLUTE Interference screw |
Biosure interference screw |
 |
 |
 |
 |
| From Benjamin, 1994 |
Image © Smith & Nephew. Used with permission. |
From DePuy-Synthes. © DePuy Synthes 2016. All rights reserved. ABSOLUTE™ is a trademark of DePuy Synthes. |
Image © Smith & Nephew. Used with permission. |
 |
| Dynamic compression hip screw |
Dynamic compression hip screw, partially threaded cannulated cancellous fixation screw and washer |
Dynamic compression hip screw
|
 |
 |
 |
 |
| There is also a partially threaded cannulated cancellous fixation screw. |
|
|
|
 |
| Herbert screw |
Herbert screws |
Herbert screw |
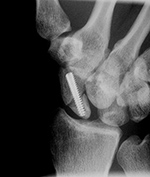
Acutrak screw |
 |
 |
 |
 |
| Note the different screw pitch on each end. From Benjamin, 1994
|
Also know as headless (recessed) fixation screws. From Taljanovic, 2005 |
There is a healing scaphoid fracture, and a fiberglass splint is in place. From Benjamin, 1994 |
The Acutrak screw stabilizes a scaphoid fracture. |
 |
| Accutrak screws
|
Dynamic compression plate and syndesmotic screws as well as two fully threaded cortical medial malleolus screws
|
 |
 |
 |
 |
| The Accutrak screws are used for arthrodesis of the distal interphalangeal joints of the right index and long fingers in a woman with severe osteoarthritis.
|
|
|
Back to Top
|