|
|

|
Orthopedic medical devices and cross-sectional imaging:
protocols and artifacts continued
by David Melville, MD
Magnetic Resonance Imaging Protocols continued
| Table 2: Sample Metal Artifact Reduction MR Imaging Protocol |
| Sequences: |
|
|
|
| T1 FSE: |
Axial |
Sagittal |
Coronal |
| STIR: |
Axial |
Sagittal |
Coronal |
| |
|
|
|
| Positioning: |
Long axis of hardware along magnetic field |
|
| Scanning: |
Frequency gradient direct away from region of interest, employ FSE and wide receiver bandwidth (16 or 32) |
| Matrix: |
512 x 512 |
|
|
| Do not use: |
Intravenous contrast, gradient echo sequences, standard fat-saturation |
| If available: |
Use proprietary metal artifact reduction techniques (MAVRIC, SEMAC) |
| Figure 21A |
Figure 21B |
Figure 22 |
Figure 23A |
 |
 |
 |
 |
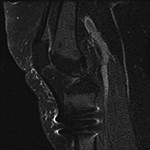
Susceptibility Artifact. (A) Sagittal proton-density-weighted fat-saturated image of the knee shows susceptibility artifact arising from three metallic screws for patellar tendon transfer with obscuration of the patellar tendon insertion and proximal tibial marrow.
(B) Sagittal proton-density-weighted image of the knee shows blooming dark signal (arrow) secondary to intra-articular gas following traumatic arthrotomy. |
Failed fat-suppression. Coronal T2 fat-saturated image of the ankle with extensive susceptibility artifact due to distal fibular plate and screws shows failed marrow fat suppression involving the distal tibia and hindfoot with demarcation between successful (arrow) and failed suppression in the talus (curved arrow).
|
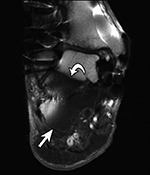
Inversion Recovery Imaging. (A) Axial spectral adiabatic inversion recovery (SPAIR) image used during MR examination of the abdomen and pelvis demonstrates large regions of susceptibility due to bilateral metal-on-metal hip arthroplasties as this technique is highly sensitive to field inhomogeneities.
|
 |
| Figure 23B |
Figure 24A |
Figure 24B |
Figure 25 |
 |
 |
 |
 |
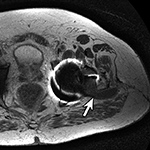
| Inversion Recovery Imaging. (B) Axial STIR MR image in the same patient reveals fluid-signal pseudotumor (arrow) adjacent to the left greater trochanter, which was obscured on prior examination. |
Adverse reaction to metal debris with posterior pseudotumor. Axial T1-weighted fast spin echo (FSE) (A) and STIR (B) MR images demonstrate left peritrochanteric fluid collection (arrow in A and arrowheads in B) arising from the left hip joint in a patient with metal-on-metal hip arthroplasty. Note the thin low T2 signal rim surrounding the fluid collection representing metal deposition. |
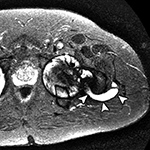
Adverse reaction to metal debris with anterior pseudotumor. Axial T1-weighted MR image shows large soft tissue mass (arrowheads) centered at the level of the lesser trochanter with involvement of the iliopsoas attachment site in a patient with metal-on-metal hip arthroplasty. Also note infiltrative involvement of the rectus femoris muscle.
|
Back to Top
Applications of MRI
As with CT, MRI can be performed to assist in the evaluation of infection, mechanical loosening, hardware failure or periprosthetic fractures. While CT is the preferred cross-sectional imaging technique for investigating osseous anatomy, MRI provides more detailed assessment of soft tissue structures. Familiarity with common post-operative indications for MRI allows the interpreting radiologist to tailor the examination to adequately assess the structures of interest and to refine the search for post-operative complications.
Adverse Reaction to Metal Debris
Metal-on-metal hip arthroplasties were initially introduced in the 1930s, but fell out of favor with the introduction of metal-on-polyethylene hardware (Ostlere, 2011; Wiles, 1958). The unsatisfactory long-term results of metal-on-polyethylene implants in younger patients, specifically related to liner wear and associated small particle disease, have led to a resurgence of metal-on-metal prostheses with improved design (Ostlere, 2011; Sochart, 1997). However, hip arthroplasties with metal-on-metal components are subject to unique post-operative complications owing to implant composition and biologic response (Hayter, 2012).
Metallosis results from shedding of large quantities of metallic debris. It is more common in metal-on-metal hip arthroplasties but may also occur following failure of polyethylene liners. This condition results in cloud-like regions of opacity on radiographs, and hip aspiration will reveal oily, black fluid (Bestic, 2013).
Another adverse reaction to metal debris is described histologically as aseptic lymphocyte-dominated vascular-associated lesions (ALVAL), a delayed hypersensitivity response to metal particles. Affected patients will present as early as a few months following surgery with a painful palpable mass, which may be accompanied by femoral neuropathy (Clayton, 2008). This condition is associated with regions of adjacent tissue necrosis of varying size believed secondary to ingestion of microscopic cytotoxic metal particles by macrophages (Ostlere, 2011; Mahendra, 2009). These reactive lesions can appear predominantly solid with regions of necrosis, mimicking the appearance of a malignant neoplasm, thus leading to the descriptive term “pseudotumor” (Pandit, 2008).
The formation of periprosthetic pseudotumors is now recognized as a major cause of metal-on-metal hip arthroplasty revision and raises long-term safety concerns about such implants (Ostlere, 2011). The risk factors for developing a pseudotumor include female sex, small prosthetic cup size, poor component positioning and sizing with increased frequency in large femoral head implants, as well as 33% chance of contralateral pseudotumor in bilateral resurfacing arthroplasties (Ostlere, 2011; Grammatopoulos, 2010; De Haan, 2008; Glyn-Jones, 2009). Elevated serum and intra-articular metal ion levels (cobalt and chromium) are associated with this condition, and it is important to correlate the imaging findings with the patient's laboratory parameters (Kwon, 2011).
On MRI, pseudotumors will appear as solid, cystic or mixed masses adjacent to and possibly communicating with the hip joint with potential intralesional or peripheral low T2 signal, reflecting metal deposition (Figure 24) (Chen, 2011). Solid lesions more commonly occur anteriorly, usually within the psoas muscle and may extend proximally into the pelvis (Figure 25) (Ostlere, 2011). Predominantly cystic lesions typically arise from the posterior joint space and may or may not demonstrate wall-thickening. Lateral lesions usually involve the trochanteric bursa and often communicate with the joint space. Differentiation of cystic and solid lesions may be difficult and the use of post-contrast imaging is not helpful for lesion detection, particularly due to surrounding metallic artifact. There may be involvement of the adjacent osseous structures with associated erosions, as well as the soft tissues, particularly the gluteal tendon attachments with resulting tendon disruption and muscle atrophy (Figure 26) (Anderson, 2011). In rare cases, the reactive process may involve pelvic or lower extremity arteries or the femoral nerve, particularly when occurring anteriorly (Clayton, 2008; Chen, 2011). At present, there is no established pathway for the management of metal-on-metal pseudotumor patients, and follow-up imaging may be performed to assess lesion progression before proceeding to revision, especially with small lesions or minor symptoms.
Back to Top
Back to top
Ultrasound
Ultrasound is a useful tool in evaluating soft tissues adjacent to metallic orthopedic hardware. While evaluation of the bone and other structures immediately deep to metallic implants may be limited, the surrounding soft tissues are typically well visualized. Ultrasound is an inexpensive, readily available imaging technique allowing dynamic evaluation.
This technique can be used to evaluate for pseudotumor in metal-on-metal implants with rapid assessment of anterior, posterior, and lateral aspects of the hip to identify heterogeneous, hypoechoic masses with no or minimal intralesional vascularity on Doppler ultrasound (Figure 27) (Chen, 2011). It is also useful for evaluation of the rotator cuff in patients with prior cuff repair or proximal humerus fracture fixation (Figure 28), as well as for assessment of ankle tendons in patients with persistent pain following fracture fixation.
|